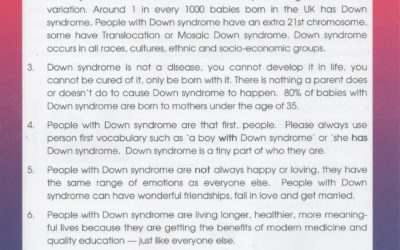
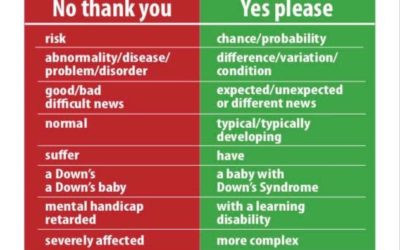
The NHS is considering introducing a new test for pregnant women that will make it much easier to detect and search out any babies with Down Syndrome (DS) or other chromosomal differences.
A superficial reading of new screening recommendations suggests that implementing new tests will save lives – and money too. It will give mothers more choice and will be safer. The statistics cited in the recommendations back this up. Except that the report cited completely ignore another set of figures that tell a rather less palatable story.
There has been some cursory coverage in the media on these new tests for pregnant women which can more easily detect babies with DS. Non-invasive prenatal testing (NIPT) makes use of cell-free DNA (cfDNA) from the baby circulating in the mother’s blood and is more accurate and safer than most other pregnancy screening tests. Hence the detection of a higher proportion of babies with DS. Because it is more accurate, fewer women will have invasive amniocentesis tests, which carry a small risk of miscarriage.
At the moment, the NHS is likely to implement NIPT into the national screening programme. The benefits, it is claimed, are that it will increase the number of DS cases detected. It: ‘…should not add significant extra cost to the screening programme’ and the number of (healthy) babies lost through miscarriage will fall dramatically.
In other words, more ‘healthy’ babies ‘saved’ and more babies with DS ‘detected’.
Other statistics tell the rest of the story.
Figures also prepared for the NHS’s consultation, by the RAPID evaluation, are notfully cited in the NHS consultation (I wonder why).
The RAPID figures project that that the proposed tests would result in 102 more babies with DS being detected each year. Therefore, based on the current 90 per cent of parents with a diagnosis that terminates their pregnancy, this will result in92 more babies with DS being aborted each year.
Allowing for the reduced number of inadvertent miscarriages of ‘healthy’ babies (down by 25), this would lead to an overall increase in fetal loss of 66 per year(but a saving of £337,000).